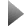having a 2.3-fold higher prevalence compared to males (9). Previous studies show a similar high prevalence among adolescents, but these studies have been done in select sports populations. This is surprising and shows that PFP does not only exist among adolescents involved in sports.
OF 7%, WITH FEMALES HAVING A 2.3-FOLD HIGHER PREVALENCE COMPARED TO MALES
100
80 90
70 60 50 40 30 20 10 0
l l l PFP No knee pain l l
TO OUR SURPRISE WE FOUND A PREVALENCE
Pain Symptoms ADL
Sport/rec
QOL
Figure 2: Knee injury and Osteoarthritis Outcome Score for adolescents with patellofemoral pain (PFP) compared to adolescents with no knee pain. (M.S. Rathleff, 2014)
3 2.5 2 1.5 1 0.5 0
One third of adolescents with PFP in our large population-based study did not participate in leisure time sports outside of school. However, those involved in leisure time sports participated a median of 5 times per week. Interestingly, frequent sports participation is a risk factor for persistent knee pain among young adolescents (10,11). This suggests that activity level may be a very important factor as PFP is probably the result of excessive loading of the patellofemoral joint caused by physical activity or structural mal-alignment of the patellofemoral joint (8, 12). In our population-based cohort, adolescents between 15 and 19 years old with PFP had a median symptom duration of more than 3 years (38 months). They reported severe pain and had a low quality of life [see example of Knee Injury and Osteoarthritis Outcome Score (KOOS) in Fig. 2]. For comparison, the KOOS subscores resemble those of elderly patients (mean age 71.3 years) 6 months after total knee replacement (13), whereas the KOOS pain and KOOS symptoms scores resemble those of young female patients (mean age 25 years) waiting for primary anterior cruciate ligament recon¬struction (14). This highlights that PFP is a significant problem for the adolescents. Among a subgroup of 57 adolescents with PFP, we compared the neuromuscular control during stair descent and isometric knee extension strength to a group of 22 adolescents with no knee pain. The results showed that adolescents with PFP had significantly lower isometric knee extension strength (Fig. 3) (15). The primary implication for this is that we should not only try to target control or strength in our exercise therapy. We need to target both control deficits and strength deficits as both are being reduced.
Furthermore, we compared PFP No knee pain
Figure 3: Isometric knee extension strength among adolescents with PFP compared to adolescents with no knee pain. (M.S. Rathleff, 2014)
22
pressure pain threshold around the knee and lower leg among a subgroup of 57 female adolescents and compared them to 22 adolescents with no knee pain. Most interestingly, they had reduced pressure pain thresholds around the knee and lower leg, indicating local and spreading sensitisation of the central nervous
pain system (9). This is important, as it indicates altered processing of nociceptive information in female adolescents with PFP, and the likelihood that both peripheral and central mechanisms may facilitate their pain. The primary implication for this finding is that sometimes we may need to think outside the box and not only focus on biomechanics and strength factors. If the adolescent show signs of central sensitisation it might be important during the initial phase of rehabilitation to consider general exercises not involving the knee and to focus on self-management and education. Collectively, this highlights that PFP is a problem from both a self-reported point-of-view as well as shown by more objective measures of strength, neuromuscular control and pain.
TREATMENT OF ADOLESCENT PATELLOFEMORAL PAIN There is no question that adolescent PFP is a significant problem, but how should we treat it? Among adults with PFP, exercise therapy is the cornerstone and offers superior effects compared to patient education or wait-and-see (16,17). However, both patient education and wait- and-see approaches are used in general practice and so far only a single study has compared patient education to exercise therapy (17). It showed better outcomes at 3 and 12 months among mostly adult patients randomised to exercise therapy (17). No studies have been conducted among adolescents with PFP which hampers evidence-based treatment of troubled adolescents with PFP. Therefore we started a project in 2010 to investigate the effect of exercise therapy as an add-on therapy to patient education compared to patient education alone on self-reported recovery. We conducted a cluster-randomised study and recruited adolescents from a closed population-based cohort (four upper secondary schools) consisting of 2,200 adolescents between 15 and 19 years. We randomised 121 adolescent with PFP to either: (1) patient education alone, or (2) patient education combined with exercise therapy.
sportEX medicine 2014;61(July):21-25
Maximal quadriceps torque (Nm/kg)
Knee injury and osteoarthritis outcome score
 Previous Page
Previous Page